Assisted reproduction techniques help thousands of couples with infertility to circumvent their problem and become parents. Nevertheless, when it is not possible for a woman to conceive due to poor egg quality or from having no eggs at all, she may still become pregnant by using eggs from a donor.
The first pregnancy with egg donation was reported in 1983, and ever since, more and more women are choosing this procedure to achieve their dream of having children. The main reason for this trend is that women are increasingly postponing childbearing until later on in life, when their fertility is often reduced; another reason is that over the years, the process has become highly successful due to recent technologies advances and improved freezing techniques.
What is egg donation?
Egg donation is a form of assisted reproduction by which a woman donates her ova to enable another woman to conceive. These oocytes are fertilized by the recipient’s husband sperm, or alternatively by a donor sperm.
The resulting embryos are transferred into the recipient uterus, which has been adequately prepared to receive them. The difference with routine in vitro fertilization (IVF) is that the egg donor is not the recipient; that is, they are two different women.
If pregnancy occurs, the recipient will have a biological but not a genetic relationship to the child, and her partner (if he provided the sperm) will be both biologically and genetically related.
What are the indications for egg donation?
 Egg donation may be considered in the following situations:
Egg donation may be considered in the following situations:
- Premature ovarian insufficiency: a condition in which menopause begins earlier than usual, usually before the age of 40 years old. In most cases the cause is unknown, but it may be the result of certain diseases, chemotherapy, radiotherapy or surgical removal of the ovaries. Egg donation is also suitable for women who were born without ovaries.
- Low ovarian reserve: when there is a decrease in the number of eggs, resulting in reduced chances of pregnancy. Generally, this is due to advanced reproductive age, as the number of oocytes -and therefore fertility- decreases rapidly after the age of 35-40 years old.
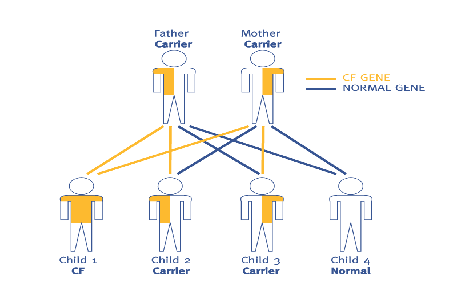
- Genetically transmitted diseases: women affected by, or carriers of a significant genetic disease who would prefer not to pass this disease on to their child.
- Previous history of failure with IVF: especially when egg quality seems to be the problem.
Who are the egg donors?
 1) Anonymous, voluntary donors: According to the Greek law, candidate egg donors are covered by anonymity and are required to sign a specific consent for the donation of their genetic material. In order to accept a woman into an egg donation program she should meet the following requirements:
1) Anonymous, voluntary donors: According to the Greek law, candidate egg donors are covered by anonymity and are required to sign a specific consent for the donation of their genetic material. In order to accept a woman into an egg donation program she should meet the following requirements:
- Age between 18 and 35 years old.
- She should be healthy, non-smoker, with no personal or family history of genetic diseases.
By law, the donor receives financial compensation only for the loss of working days, travel and other expenses incurred during the treatment cycle in which she participates. In any case, egg donation is an altruistic, anonymous and voluntary act.
2) Egg sharing: Women undergoing IVF may agree to donate their surplus oocytes to other women with infertility.
3) Known donor: a person who is known to the recipient, usually a close relative of friend. According to the Greek law, oocyte donation is an anonymous procedure, that is, the donor has no access to the child born, nor the recipient to the donor. Therefore, in Greece the donation of ova to known persons is forbidden by law.
Evaluation of the egg donor

Each candidate donor, after being fully informed about the egg donation program, completes a thorough questionnaire on her family, medical and psychological history. In addition, she is the subject of a series of exams to determine whether her health is in good condition and she can respond properly to the hormonal therapy.
The evaluation involves a comprehensive physical and gynecological examination, as well as the assessment of her psychological and mental status, her genetic material and reproductive system.
In addition, donors undergo the following laboratory testing:
- Blood type and Rhesus
- Hepatitis B & C
- HIV 1 & 2
- Syphilis
- Hemoglobin electrophoresis
- Sickle cell trait testing
- Cystic fibrosis (CF) mutation
- Fragile X testing
- Conventional karyotype. It is also possible to a perform a molecular karyotype, upon request of the recipient couple.
A donor is ineligible if either the questionnaire or the screening tests indicate the presence of risk factors, or clinical evidence of an infectious or genetic disease.
Evaluation of the recipient couple

Adequate screening and preparation of the recipient couple are essential for the success of an egg donation program.
According to the Greek law, a woman is considered suitable to receive oocytes when her uterus has normal morphology and functionality and has not exceeded the age of 50 years.
The evaluation of the recipient couple is similar to that of couples undergoing routine IVF. First, the physician obtains a thorough medical history from both partners.
The assessment of the woman includes an in-depth physical and gynecological examination, a detailed pelvic ultrasound and laboratory testing. Briefly, the ovarian function, her blood group, and exposure to certain infections are examined. In addition, a Pap smear test and cultures for certain microbes (Neisseria gonorrhoeae, Chlamydia trachomatis, etc) are obtained.
In some cases, the uterine cavity is evaluated with hysterosalpingography (HSG), sonohysterography or hysteroscopy. If the woman is over 45 years old, a more thorough assessment of her cardiac function, pregnancy-induced hypertension and gestational diabetes risk are recommended. The effect of advanced maternal age on pregnancy will be discussed extensively, as well as any medical conditions that may affect pregnancy.
An embryo transfer trial before the actual procedure (“mock” embryo transfer) is strongly recommended. It allows to determine the best way to place the embryos into the uterus, and ensures that there are no unexpected obstacles along the way. Sometimes the cervix is very narrow and hinders the transfer of the embryos into the uterus; this may result in significantly reduced chances of pregnancy. In case of a narrow or distorted cervical canal, a cervical dilation may be recommended.
A treatment trial in a previous cycle with the same medications used for the endometrial preparations is proposed when possible, in order to assess the uterine response to hormone therapy.
The male assessment includes a semen analysis, blood group and genetic testing, among other exams.
According to the Greek law, the recipient couple should be tested for syphilis, hepatitis B and C, HIV-1 and HIV-2 within the six months preceding the treatment cycle.
The procedure
Preparation of the donor for egg retrieval
The donor follows the procedure of a standard IVF. Initially, she undergoes ovarian stimulation, that is, she receives a combination of hormonal medications in order to achieve the development of a sufficient number of oocytes within the ovaries; egg development is monitored by ultrasound and blood exams at regular intervals. When the oocytes are at the appropriate size, ovulation is triggered by an injection of human chorionic gonadotropin (hCG). Oocyte retrieval, scheduled approximately 34-36 hours after hCG administration, entails the use of a needle which is inserted through the vagina into the ovaries, whereby the eggs are aspirated under ultrasound guidance. The procedure is carried out under a mild sedation.
The ova obtained are evaluated for their maturity and then fertilized with the partner’s sperm, which has been processed in the laboratory. Donor sperm may be also utilized when indicated.
The male partner should provide the semen sample the day of the donor’s egg retrieval. Alternatively, if the presence of the partner is not possible on that day, the semen can be cryopreserved (frozen) at an earlier time.
Preparation of the recipient for embryo transfer
In order for the embryos to implant into the recipient’s uterus, the endometrium (uterine lining) must be prepared and synchronized with the donor cycle.
There are numerous protocols for endometrial preparation. Briefly, women who still have menstrual period may receive an injectable medication for temporary suppression of the ovarian function. When the donor starts ovarian stimulation, the recipient receives a hormone called estradiol to achieve endometrial growth. Estradiol can be administered orally or through a transdermal patch. Ultrasound assessment of endometrial thickness -and occasionally blood tests- are performed during this period. On the day after the donor receives hCG, the recipient begins treatment with progesterone. Progesterone causes endometrial maturational changes that allow the embryo to implant. Progesterone can be administered by intramuscular injection, vaginally or orally. Besides estradiol and progesterone, other medications may be prescribed if required.
The embryos are transferred into the recipient’s uterus, usually within three to five days after fertilization of the eggs in the laboratory. Embryo transfer is done using a thin catheter inserted through the cervix into the uterus. If the recipient couple has extra embryos, they will be cryopreserved (frozen). Thus, it is possible to transfer these embryos at a later time without the need for another egg donation.
Hormonal therapy with estradiol and progesterone continues until the recipient takes a blood pregnancy test (β hCG). If the test is positive, the hormones are continued during the first trimester of pregnancy.
Success rates with egg donation
Since egg donors are young and healthy women, success rates are higher than those obtained with conventional IVF. The age of the recipient does not seem to affect the success of the procedure. According to data from the National Agency of Medically Assisted Reproduction, the pregnancy rate with egg donation in Greece is 54%.
Nevertheless, the greater the number of attempts with donor-egg IVF, the higher the odds of success. Thus, it is estimated that the success rates after the third attempt reach almost 90% in most cases.
Many factors play an important role in the success of the procedure: adequate evaluation and preparation of both donors and recipients, optimal synchronization between them, high laboratory standards and well-trained scientific staff, will all have a positive impact on pregnancy rates in an egg donation program.
Risks of egg donation
1) For the donor:
Egg donation is a very safe procedure. Nevertheless, it is not entirely risk-free. Medicines taken to stimulate the ovaries, oocyte retrieval and the anesthesia required are all possible sources of complications. Briefly, the side effects of medications are usually mild, as one of the most feared complications in assisted reproduction, ovarian hyperstimulation syndrome is very rare in these cases. The remaining risks are estimated as follows: anesthesia risks: 1 / 10,000; risk of severe bleeding from oocyte retrieval: 1 / 2,500; risk of infection: less than 1/500.
It should be noted that the fertility of women who become egg donors is in no way affected. In fact, the eggs donated would have been otherwise discarded by their bodies.
2) For the recipient:
The possibility a donor transmits an infectious disease to the recipient is virtually non-existent, provided that proper evaluation of the egg donor has been performed, as dictated by the Greek law.
The most common risk for the recipient is the occurrence of a multiple pregnancy (twins) if more than one embryo is transferred. In any case, in egg donation cycles, the transfer of more than two embryos is strictly forbidden by the Greek law. If the couple is opposed to the possibility of a twin pregnancy, then only one embryo may be transferred (single embryo transfer, SET).
Pregnancy complication risk in recipiens with advanced age should be assessed individually for each case.
3) For the child:
To date, thousands of children have been born with this procedure, and the available data is reassuring, and equivalent to that of conventional IVF: the rate of birth defects is the same as the general population.
THE LEGISLATION IN GREECE
On Egg Donation
- Egg donation is an altruistic act, voluntary and with no financial benefit. Donors are compensated only for the working days they lose as part of the donation process and their travel expenses.
- Donation of ova and sperm is allowed in Greece provided donor anonymity is ensured.
- Egg donation is not allowed to women over 50 years old.
- Donors must sign an oocyte concession consent.
- Recipients sign a document stating that they are married and accept to undergo in vitro fertilization with egg donation. If they are not married, they should sign a notary act stating that they wish to undego IVF using the egg donation method.
On Assisted Reproduction
On January 27 2005, the law 3305/2005 on the application of assisted reproduction techniques was reported.
The Greek law on medically assisted reproduction is one of Europe’s most flexible. It safeguards the couple who wants to have a child based on medical, biological and bioethical principles. Its main purpose is, ultimately, the protection of the child to be born.
Basic principles of the current legislation
Some of the key points of the in-force law are the following:
1) Assisted reproduction methods are legal and allowed for women up to the age of 50 years, as this is considered the limit for natural conception.
2) The donation of ova and sperm is permitted, but the consent of the spouse or partner is also required.
3) Pre-implantation genetic diagnosis is allowed with the purpose of diagnosing whether the resulting embryos are carriers of genetic diseases. Consent of the concerned individuals is required.
4) Sex selection is prohibited unless a serious sex-related hereditary disease is avoided.
5) Cloning for reproductive purposes is prohibited.
6) Cryopreservation of genetic material or fertilized eggs is permitted.
7) The use of a gestational carrier (surrogacy) is allowed. A surrogate is a woman who carries a pregnancy for another couple or woman, who wishes to have a child but is unable to get pregnant for medical reasons. The surrogate woman must undergo medical and psychological examination. There should be no financial transaction other than the costs resulting from pregnancy exams, loss of work, etc. The procedure requires a special permit from a judge.
8) Assisted Reproduction Units are established and operate with the permission of the competent Authority, which shall give its agreement and verify that the legal requirements are met. For any violation, it sets administrative and criminal penalties.
9) The law sets age limits for sperm donors (younger than 40 years old) and egg donors (younger than 35 years).
10) Single women are allowed to conceive with assisted reproduction.
11) Donors must undergo clinical and laboratory testing and are not admitted to donation programs if they suffer from hereditary, genetic or infectious diseases. The use of fresh semen from donor is not permitted; only frozen semen may be used.
More info at gofertile.eu